Dentures
Removable dentures (sometimes referred to as false teeth or plates) are a common treatment alternative for missing teeth. Removable dentures are versatile in their ability to replace any number of missing teeth and to fill out the contours of the face and lips, which shrink inward when multiple teeth are lost. Typically the denture base is made of acrylic plastic that can be tinted to match the patient’s natural gum tissues. The teeth are made from either acrylic or ceramic.
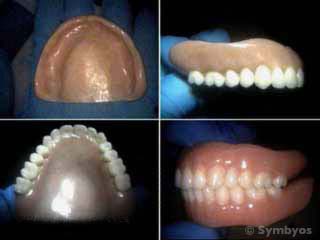
Figure 1: Different views of a removable complete denture.
Figure 1 shows different views of a complete removable denture for the patient’s upper jaw (maxilla). The upper left photograph shows the side of the denture that is worn against the patient’s gums, where their teeth used to be. Note that the denture base (the pink part that holds the teeth and rests on the gum tissues) covers the roof of the mouth (palate), and adds bulk on the side towards the lips and cheeks to give the face proper contours. The lower right photograph shows how the denture will function with the patient’s lower denture. Ideally, upper and lower dentures are made in sets for patients with no teeth (completely edentulous). This provides the best chewing efficiency and esthetics.
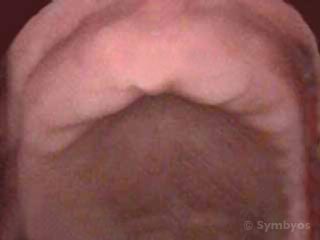
Figure 2: Complete tooth loss (edentulism) of the upper jaw (maxilla) requiring a removable complete denture.
Complete removable dentures are an option if you are missing all of your teeth, while partial removable dentures (partials) are an option if you are only missing some teeth. Partial removable dentures are held in place in the mouth by wire clasps and/or other means of attachment to the remaining natural teeth. Partial dentures can be a temporary means of treating patients who are expecting to lose the remaining teeth. As more teeth are lost, they can be added to the partial. At some point, as the natural teeth being used to anchor the partial denture (abutments) are lost, it becomes necessary to completely remake the denture, or explore other treatment options, like dental bridges or dental implants—both of which are usually good solutions for the replacement of single teeth as well.
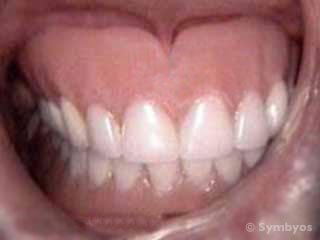
Figure 3: The removable dentures shown in the previous photograph are shown here in the patient’s mouth. The lips are being retracted for the photograph. Note that the dentures fill the space left by the missing teeth and shrunken underlying bone and gum tissues, to provide the correct amount of vertical spacing between the upper and lower jaws, and to fill out the cheeks and lips.
Complete removable dentures are held in place by some combination of “suction cup effect”, denture adhesive (best if used very minimally), and the patient’s controlled use of their tongue and facial muscles. Learning to function with complete removable dentures can be a challenge, as with any prosthetic device. Dental implants can also be used to help stabilize dentures, and often significantly improve a patient’s quality of life.
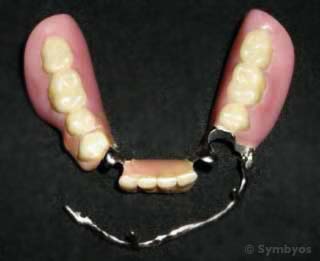
Figure 4: A swinglock partial removable denture is one option for tooth loss. This one is for the lower jaw.
Figure 4 shows a partial removable denture for the lower jaw (mandible). Note that the denture replaces all but three of the patient’s natural teeth, which will be used to retain the denture in place in the mouth. This denture has a swing lock clasping feature, consisting of a hinged bar, shown in the open position. The swing lock will not be visible behind the patient’s lower lip when the denture is placed in the mouth. The ability to remove the denture makes it much easier to clean such retention features. Not evident from the photograph is that the metal framework which serves as the denture’s skeleton extends under the pink plastic gum tissue and denture teeth to strengthen them. Generally the framework is made of an extremely hard nickel-chrome alloy; however, for those with nickel allergies, other materials can be used.
See also on ToothIQ.com