Dental fillings
Fillings are among the most frequently prescribed and versatile of all dental restorations. In a procedure known as cavity preparation, the dentist uses any of a variety of dental drills (also called burs), microabrasion devices, or laser tips to remove damaged tooth structure, and any tooth material that has been weakened or undermined by decay. Applying their knowledge of ideal tooth shape, dentists replace the missing tooth structure with filling material of various types.
Fillings are placed into teeth following the removal of dental caries (cavities/tooth decay), and filling material can also be used to restore chipped or partially broken teeth to their normal contour and function.
When performed traditionally, a mixture of silver, zinc, copper and mercury known as amalgam is used to fill the back teeth, and sometimes even the front ones if the decay is on a surface that is not visible when the patient smiles. Although they can be bonded into the tooth with modern dental adhesives, silver fillings are held into the tooth primarily by mechanical interlocking features cut into the tooth by the dentist.
If replacement of multiple silver fillings is recommended, it’s a good idea to understand what’s involved and why it’s important. Diagnostic photographs of failing (for example, cracked) fillings can help you to understand why replacement may be needed. If you are having it done for cosmetic reasons, it’s important to understand the risks.
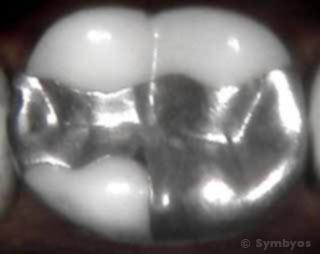
Figure 1: A large silver filling in a lower molar tooth. (Image courtesy Byron J. Greany, DDS)
Figure 1 shows a large silver filling in a lower molar tooth. These fillings have been the workhorse of dentistry for many years, and when properly placed and cared for, can provide decades of service. Placing silver fillings in the presence of significant moisture (for example, saliva) can cause them to outgas, resulting in pitting and voids that reduce their service life. That’s why it’s important to isolate the teeth with a rubber dam or cotton rolls when placing silver fillings in them.
The debate surrounding the use of mercury in silver fillings continues. Because of silver amalgam’s durability, track record for long term success, ease of use, similar wear properties to natural tooth enamel, and relative inexpense, it continues to be widely used and endorsed as safe for most patients. If you have questions about the safe use of silver for you or your child, talk it over with your dentist. There are generally other options available.
Beginning in the 1960’s a process known as dental bonding was developed. Since its inception, dental bonding has continued to improve in strength and durability, allowing teeth to be more conservatively restored. Modern bonding materials may allow teeth that have been structurally compromised to be repaired with long-lasting and cosmetically pleasing fillings. A tooth-colored material known as composite resin is currently used to restore many cavities—even those found in the back teeth (Figures 2, 3, and 4).
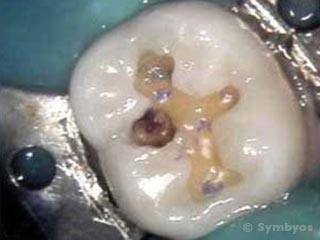
Figure 2: Tooth decay (caries) has created a cavity in this partially prepared lower molar tooth.
Figure 2 shows where dental caries created a cavity in this partially prepared lower molar tooth. Blue caries detection dye has been used to identify less obvious areas of decay. Use of caries detection dye helps the dentist remove all of the decay without removing too much tooth structure.
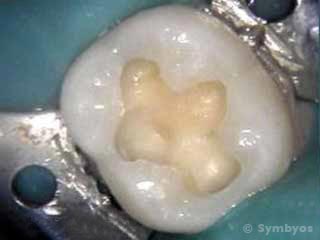
Figure 3: The decay has been removed.
Figure 3 shows the cavity prepared for a filling. The decay has been removed, and the preparation stained with dye to verify complete caries removal. No dye is visible, because the decay has all been removed. If the decay is very deep into the tooth, the dentist may place a layer of base material (an insulation layer) over the yellow dentin floor. Some cavities require very thin base layers called liners.
Bases and liners can reduce post-operative sensitivity in the tooth, and promote formation of reparative dentin (a calcified substance cells in the tooth produce to protect the pulp from damage). Some dentists apply desensitizing agents to the exposed dentin before filling the cavity. All of these techniques are considered to be part of the filling process.
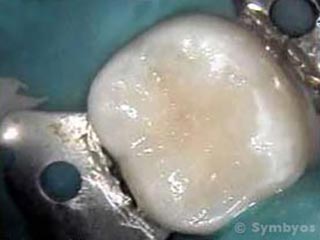
Figure 4: A tooth-colored composite resin filling has been placed in the prepared cavity.
In Figure 4, a tooth-colored composite resin filling has been placed in the prepared cavity. Well placed and well taken care of, it should provide many years of service.
See also on ToothIQ.com